Sciatica
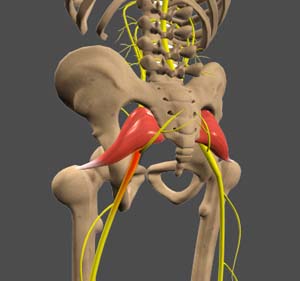
What is the Sciatic Nerve?
The sciatic nerve is found in the lower back and runs down the leg. There is one on the right and one on the left. It is rare the sciatic nerve itself is irritated, but more commonly, it is nerves that make up the sciatic nerve that is compressed. Typically, the nerves at L4, L5, and/or S1 are affected.
What is Sciatica?
Sciatica is a painful generic term indicating irritation of the sciatic nerve. Sciatica is typically caused by a herniated disc in the lower lumbar spine. Sciatica can be acute (short term), lasting for a few weeks or chronic (long term), persisting for more than 3 months. Majority of people (70%) will get better with time in the first 2-3 months. If it does not improve significantly after that, typically surgery is a faster, better option.
Symptoms of Sciatica/Herniated disc
The most common symptom of a herniated disc is pain. The pain can vary from mild to debilitating depending on the degree of pressure exerted on the sciatic nerve. Patients having nerve compression experience other symptoms such as:
- Pain in the buttock area and leg
- Sharp, intense, shooting pain down the leg
- Numbness, burning or tingling sensation in the leg or foot
- Weakness of the leg or foot
- Lower back pain that radiates down the buttock and leg
- Pain that increases with coughing, sneezing or straining
- Pain that increases with bending backward and with prolonged sitting or standing
Diagnosis of Herniated Disc
Sciatica/herniated disc is diagnosed by reviewing your complete medical history, performing a physical examination and assessment of neuromuscular functions. Advanced imaging such as MRI, CT scan, CT scan with myelogram, electromyogram, and nerve conduction tests are needed to confirm the diagnosis of nerve compression/sciatica.
Treatment of Sciatica/Herniated Disc
Herniated disc can be treated with conservative approaches such as physical exercises, over-the-counter drugs, ice or hot packs, prescription medications, epidural steroid injections, massages, and manual manipulation. These treatments do not make the herniated disc go away, but provides a means for your body to cope while your body heals the herniated disc. In many cases, a MRI done many months after a herniated will not show the herniated disc any more.
In some cases, surgery may be recommended to treat the underlying condition.
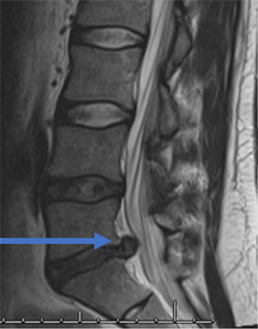
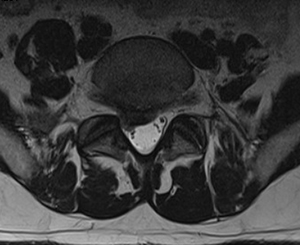
Case Study
31 year old man presents with excruciating right leg pain. MRI shows a right L5-S1 disc herniation on the right (see arrow). The left image is a sagittal view where you are seeing the spine from the side. The right image is looking at a cross section of your spine. On this view the right side is the left of the image and vice versa.
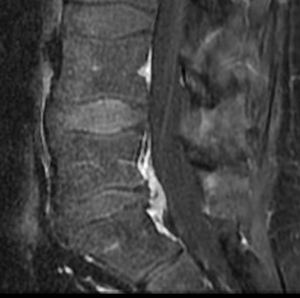
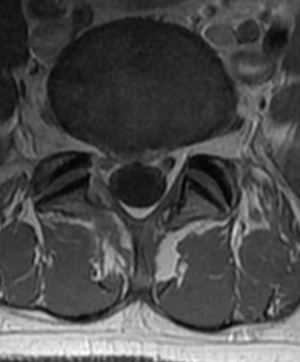
After minimally invasive surgery, the disc herniation is removed. The remaining “normal” disc is left alone.