Artificial Cervical Disk Replacement
What is Artificial Cervical Disk Replacement?
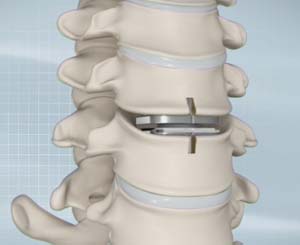
Artificial cervical Disk replacement is a spine surgery to replace a degenerated (deteriorated) Disk in the neck with an artificial Disk. The artificial Disk is similar to a knee or hip replacement. There is a titanium and plastic components.
How is Artificial Cervical Disk Replacement Performed?
For the procedure, the cervical spine is approached through an incision in the front of the neck. The affected Disk is identified with the help of imaging studies and removed. The artificial Disk is then placed precisely in the Disk space between the vertebrae. After checking the range of motion of the neck and confirming the proper fit of the artificial Disk, the incision is sutured closed.
Risks and Complications of Artificial Cervical Disk Replacement
In addition to the anesthetic complications, spinal surgery is associated with risks. Some of the potential complications associated with disc replacement include subsequent pain, impaired healing and a possible need for additional surgery. There is risk of bleeding, esophageal injury, and hardware issues (disc replacement movement/dislocation). Rarely, if bleeding continues after surgery, it can lead to difficulty breathing and possible death. It is important to have someone reliable with you at home for the few days to make sure they can check on you. There is also a risk of nerve damage, spinal cord damage, and paralysis. Since disc replacement is a relatively newer procedure, new risks, indications, and complications are emerging.
Related Topics:
- Lumbar Laminectomy
- Posterior Lumbar Fusion
- Lumbar Endoscopic Discectomy
- Minimally Invasive Lumbar Discectomy
- Anterior Lumbar Interbody Fusion
- Minimally Invasive TLIF
- Kyphoplasty
- Minimally Invasive Spine Surgery
- Oblique Lumbar Interbody Fusion (OLIF)
- Posterior Cervical Laminectomy and Fusion
- Cervical Corpectomy and Strut Graft
- Endoscopic Spine Surgery
- Surgery for Scoliosis
- Cervical Laminoplasty
- Image-Guided Spine Surgery
- Anterior Cervical Discectomy with Fusion
- Artificial Cervical Disk Replacement
- Cervical Foraminotomy
- Extreme Lumbar Interbody Fusion
